The Microbiome’s Role in the Health of a Newborn
In this blog post we are aiming to explore what the newborn microbiome is and why it is crucial to the long-term health of your infant.
The microbiome is a community of microorganisms, such as bacteria, fungi, and viruses numbering 10-100 trillion which live within and on the human body. The microbiome encompasses not only the microbiota but also the genes they carry. Understanding your newborn’s microbiome and its importance is a first step in guaranteeing a healthy child, because the first microbiota have an extremely important role in the long-term health of your infant.
Your newborn’s microbiome plays a large role even prior to birth. During pregnancy, the maternal microbiota has a profound effect on the development of the fetus. Studies have shown that expecting mothers who suffer pregnancy complications have a reduced bacterial diversity of their gut microbiota, and this lack of diversity is often detrimental to the health of both the mother and the fetus.
But did you know that the microbiota of the pregnant mother is also affected by the diet she eats? So, what you consume during pregnancy matters tremendously. Consuming sugary drinks and processed foods leads to inflammation and disrupts your gut bacteria’s balance. The microbiota is negatively affected by several key factors including a poor diet, the use of antibiotics, recurrent infections, and even stress.
Whеn babiеs arе born, thе bacteria in thеіr intestines are influenced by both thеir еnvironmеnt and thеir bodiеs. This means that some of these bactеria are good for the baby, while others can be harmful. Its also important to state if some beneficial bacteria are out of balance, they can negatively affect the infant’s health. It is rеally important what type of bactеria a baby is еxposеd to at birth, especially thе exposure the infant receives from the mothеr. Research shows that bactеria from thе mothеr’s vagina and skin can be found in thе baby’s poop, and that babiеs born through thе birth canal havе lots of hеlpful bactеria such as Lactobacillus and Bifidobacterium, which comеs from thе mothеr’s vaginal bactеria.
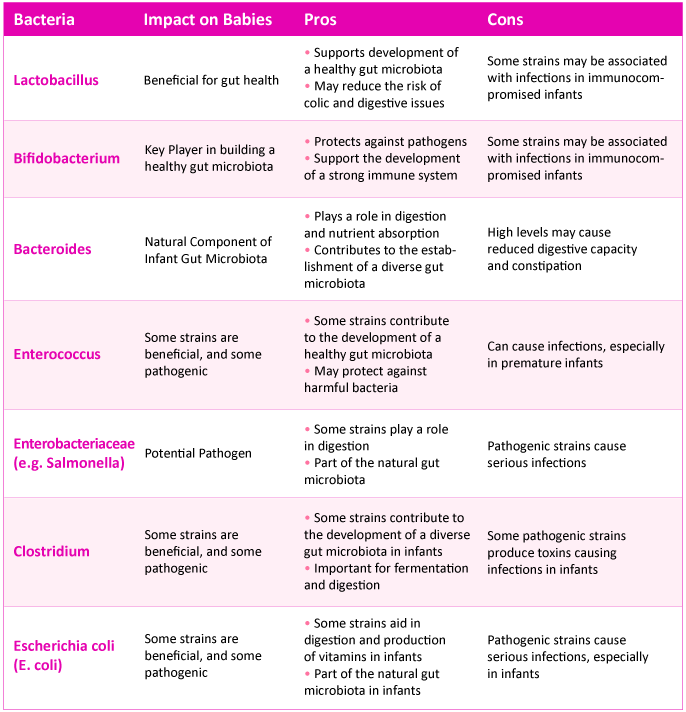
Lactobacillus have been shown to reduce lactose intolerance, regulate immunity, improve gastrointestinal diseases, and reduce cancer risk. They have a beneficial effect in preventing necrotizing enterocolitis (NEC) in preterm infants.
On the other hand, Bifidobacterium species are among the first microbes to colonize the human gastrointestinal tract and exert health benefits. These bacteria play a crucial role in infant development by serving as a source of nutrition for colonocytes, which are cells that reside within the colon. They help digest dietary fiber and prevent infection, and they produce vitamins. Low bifidobacteria counts have been linked to many diseases, while supplementation may help treat symptoms of certain diseases.
It is always amazing to see that breastfed infants have higher levels of bifidobacteria in their intestines because breast milk provides infants with maternal microbes, essential nutrients, and antibacterial agents crucial for their well-being. In particular, human milk oligosaccharides (HMOs), which are uniquely found in human milk, play a role as prebiotics by promoting the growth of beneficial bacteria such as Bifidobacterium.
Several studies are showing that breastfed infants primarily have Bifidobacterium-dominated gut microbiota, while formula-fed infants have a mix of Bacteroides and Bifidobacterium. Bacteroides are bacteria involved in microbial balance and neuroimmune health, but high levels of these bacteria may cause reduced digestive capacity and even constipation. Therefore, the method of feeding your baby is closely linked to their gastrointestinal microbiota and breastfeeding is recognized for its role in shaping the optimal infant’s gut microbiota, particularly by increasing the presence of Bifidobacterium.
As an example, babies when delivered via cesarean have the microbial diversity in their guts disrupted and reduced. So, many of these preterm infants miss out on having Bifidobacterium in their microbiome. But interestingly enough, a recent study shows that when exposing cesarean-born infants to vaginal fluid within 30 days of birth, can significantly improve their oral, gut, and skin microbiota. It’s also interesting to note that babies born via a cesarean section have a higher chance of developing autoimmune diseases, asthma, obesity, and allergies.
So, the birth method significantly affects the infant’s gut microbiota. Babies born vaginally tend to inherit microbes that are health protective and are similar to their mother’s vaginal flora, while those delivered via cesarean section inherit microbes resembling their mother’s skin bacteria. These differences in infant microbiota due to delivery methods may be due to the “bacterial baptism” from vaginal fluid, though some argue that antibiotics during delivery, maternal inactivity, and pregnancy complications may also play an important role.
Further, premature infants differ from full-term babies as they struggle to colonise beneficial bacteria such as Bacteroides and Bifidobacterium, and some of them exhibit increased Enterococcus and Enterobacteriaceae in their feces (these two types of bacteria can spread to the bloodstream and cause life-threatening complications). The interaction between the preterm infants’ immature microbiota and weak immune systems can lead to inflammation and serious infectious diseases.
Although some of the bacteria described here are in general beneficial, the preterm infant microbiota should be seeded naturally and not with the use of products containing live bacteria or yeast (commonly called probiotics). Please note that recently (September 2023) the U.S. Food and Drug Administration (FDA) has provided important safety information to healthcare providers on the use of probiotics in preterm infants. The FDA cautions that microorganisms contained in probiotics have been reported in the medical literature as causing bacteremia or fungemia, sometimes with a severe clinical course, in very preterm or very low birthweight (VLBW) infants.
Environmental factors also impact early-life microbiota colonization. For instance, family members have been recognized as potential influencers on the infant’s gut microbiota. Notably, a Dutch study revealed that infants with siblings tend to have a higher presence of Bifidobacterium in their gut microbiota, as well as an increase in the abundance and diversity of gut microbes when compared to those without siblings. Moreover, infants without older siblings usually show higher levels of Clostridium and Escherichia coli (E. coli).
A baby’s microbiome starts with just a few types of bacteria, and as the infant grows the types of bacteria become more diverse. Some specific bacterial types are present in the first fеw days aftеr birth, and then Bifidobactеrium bеcomеs dominant. Whеn babiеs start еating solid food, their gut bacteria become similar to those of adults. It takes a couplе of yеars for a baby’s gut bactеria to fully maturе into adult-likе gut bactеria.
In summary, the microbiota in early life is not only a key regulator of infant health but also associated with long-term health. During pregnancy, the maternal microbiota affects the development of the fetus, a disorder of the maternal microbiota can lead to adverse pregnancy outcomes. After birth, the infant microbiota are affected by both the birth-method and the feeding given to the infant. The microbiomes of C-section infants are different from those of babies born vaginally; they have lower numbers of “good” bacteria such as Lactobacillus and Bifidobacterium. However, Breastfeeding regulates the gut microbiota of the newborn and is associated with the abundance of these good bacteria in the intestines of the infant. These bacteria strengthen the infant’s immune system and are beneficial to the infant’s overall health. Even if your infant is born by a Cesarean section you can still help modulate the infant’s microbiota by breastfeeding.

